What are Shingles?
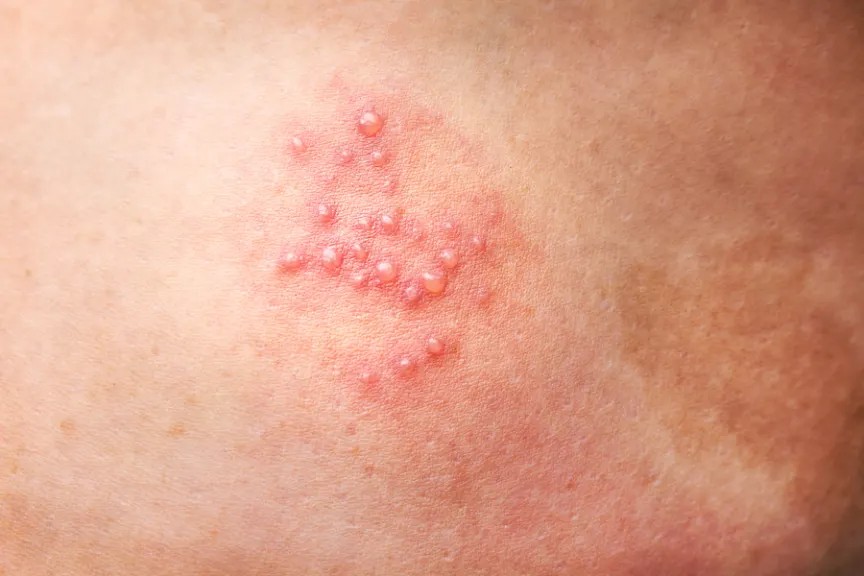
Shingles, or kayap as we Malaysians call it, is a term used to describe a cutaneous virus infection. This infection is actually a reactivation of the varicella-zoster virus which causes chickenpox. When the virus is initially introduced into the body, it can manifest as chickenpox (varicella). The virus then remains dormant in the ganglion and gets reactivated (herpes zoster) when the body is immunocompromised, usually due to advanced age, cancer, HIV infection, or usage of long-term steroids.
What are the symptoms of Shingles?
The symptoms of Shingles can be divided into 3 phases, the pre-eruptive phase, acute eruptive phase, and chronic phase.
- Pre-eruptive phase :
- This occurs about 2-3 days before the onset of the rash.
- During this phase, patients may experience non-specific symptoms such as :
- Pain
- Itchiness
- Paresthesia
- Malaise
- Headache
- Myalgia
- Fever
- What’s unique about this infection is that the pain, itchiness, and paresthesias are only felt along the specific dermatomes that are affected. The most common ones are the trigeminal and the thoracic region
- Eruptive phase :
- In this phase, symptoms from the pre-eruptive phase may still occur. Others include :
- Patchy erythema
- Regional lymphadenopathy
- Grouped herpetiform vesicles – This usually appears as clear, fluid-filled vesicles which then forms a crust that leads to scarring
- Usually, this infection would be mild in children but in adults, it can lead to severe pain.
- Symptoms usually last about 10-15 days but it can take up to a month for complete resolution.
- Chronic phase
- Also known as the post-herpetic neuralgia, this can be defined as persistent or recurring pain lasting for more than 30 days after crusting of the lesions.
- This pain also occurs along the dermatomes and is described as severe and incapacitating that can last for years. However, this is typically seen only in adults who have herpes zoster ophthalmicus or upper body dermatomal involvement.
How is Shingles treated?
Often, this infection is treated conservatively as they are usually self-limiting and may resolve on their own. However, patients can be prescribed painkillers such as NSAIDs and calamine lotion to soothe some of the symptoms. Additional treatment with neuroactive agents like amitriptyline and antivirals such as acyclovir or famciclovir can be given to reduce the risk of complications and limit the spread of the virus. Specific treatments may be necessary if the virus infection affects the eye or any other organs.
Can Shingles cause death?
Death from Shingles is not a very common occurrence, but it is possible just like any other disease, especially if the patient is already immunocompromised. While the virus may not cause death, it can lead to several complications that can lead to death. Some of them are :
- Post-herpetic neuralgia
- This is the most common complication seen in kayap. As mentioned before, the pain can be a continuation of the acute herpes zoster infection or it can recur after resolution of symptoms.
- Ramsay-Hunt Syndrome
- This can be caused by herpes zoster oticus (ear), affecting the cranial nerves 5, 9, and 10.
- Symptoms include one-sided facial weakness, ear pain, and deafness.
- Typically seen in children, rarely adults.
- Ocular complications
- Usually seen with herpes zoster ophthalmicus, it can manifest as conjunctivitis, keratitis, glaucoma, corneal ulceration, and even blindness.
- Nervous System complications
- Meningoencephalitis is usually seen in immunocompromised patients.
- Other complications are cranial nerve palsies, myelitis, or granulomatous angiitis.
- Guillain-Barré syndrome
- This complication is extremely rare, but it can be seen with primary infection of varicella-zoster virus in adults.
Vaccine for Varicella-zoster virus (Zostavax) is available in Malaysia and is recommended for adults above the age of 60 years and individuals who are immunocompromised even if they have a history of Varicella-zoster virus infection. This vaccine will not prevent the reactivation of the virus, but it can limit the severity of illness. In addition to that, it is important to refer to a doctor if you have symptoms of Kayap as prompt treatment can reduce the possibility of complications. Kayap is contagious, so if you are infected, it is best to avoid contact with those who have never been infected by this virus.












